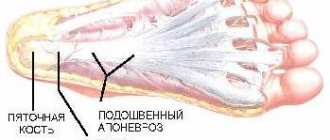
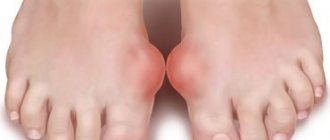
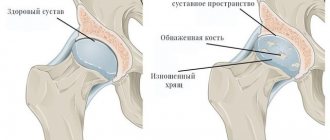
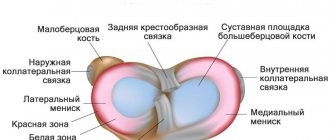
Types of polyarthritis of the joints Causes and symptoms of polyarthritis Stages of polyarthritis of the joints Treatment of polyarthritis Medicines for the treatment of polyarthritis Diet for polyarthritis
Polyarthritis
is an inflammatory disease of the musculoskeletal system that simultaneously affects 2 or more joints. With polyarthritis, several joints may suddenly become painful, or one or the other may be bothered in turn. This disease does not always affect the joints symmetrically; sometimes it can be localized in completely different parts of the body.
Polyarthritis is dangerous not only because of mobility impairments, which can lead to disability, but also because of its complications. Left untreated, it increases the risk of heart attack every year and negatively affects vision and lung function. But the question of how to cure polyarthritis and whether it can be done at all can arise before a person of any age!
Polyarthritis of the joints is an inflammatory disease that affects several joints at the same time.
Types of joint polyarthritis
Polyarthritis can affect both large and small joints of the limbs, as well as the joints of the jaw and spine. Certain types of disease may have a characteristic localization, which indirectly helps in the diagnosis of polyarthritis. For example:
- Rheumatoid polyarthritis. It is characterized by symmetrical damage to the joints, most often the wrist and interphalangeal joints, with a gradual increase in the symptoms of polyarthritis. The knee and elbow joints are often affected. Joint pain can be complemented by disorders of the nervous, cardiovascular system, vision and kidney problems.
- Reactive polyarthritis. It mainly affects the joints of the legs. The first signs of polyarthritis can appear from 2 weeks to 3 months after illness with salmonellosis, yersiniosis, mycoplasmosis, cystitis, pneumonia, bronchitis, prostatitis, pharyngitis and other infectious diseases. May be accompanied by damage to the mucous membranes and/or pain in the heart.
- Metabolic polyarthritis. It disrupts the functioning of the joints of the legs (metatarsal, ankle, knee and others), manifestations are paroxysmal in nature. Usually the disease worsens after a violation of the diet for the underlying disease.
- Infectious polyarthritis. It occurs as a result of specific infectious diseases - tuberculosis, syphilis, dysentery, brucellosis, gonorrhea - and primarily affects large joints. Pain manifests itself primarily in the shoulder, elbow, ankle, knee, and, less commonly, hip joints.
- Psoriatic polyarthritis. Despite the characteristic cause, symptoms of polyarthritis may appear before skin manifestations of the disease. It usually affects the interphalangeal joints, which gives the fingers a characteristic spindle-shaped shape.
- Idiopathic juvenile polyarthritis. Asymmetrically affects large joints, incl. cervical spine and temporomandibular.
Principles of disease diagnosis
Diagnosis of arthritis includes physical examinations by specialists, consultations with specialist doctors (cardiologist, neurologist, etc.), laboratory and other research methods.
Diagnostics consists of several parts:
Laboratory diagnostics:
General blood and urine analysis, biochemical blood test with mandatory examination of rheumatological samples. In moderate and severe forms of the disease, joint fluid is collected with preliminary puncture of the affected joint.
Instrumental diagnostics:
X-ray examination of bones and joints in 2 projections (direct and lateral) will help determine the stage and advanced stage of the process. Magnetic resonance imaging is a more accurate examination method, which is carried out to clarify the location, stage of the disease, as well as additional inclusions and lesions (erosions, growths, etc.). Ultrasound examination allows you to assess the extent of damage to the joint, the presence of fluid and the inflammatory process.
Causes and symptoms of polyarthritis
Polyarthritis can strike a person suddenly, like a bolt from the blue, or it can grow gradually, starting with completely harmless symptoms. Up to 70% of patients who sought help were older women, and their relatives already had musculoskeletal diseases. Among the most common causes of the disease are:
- infectious diseases (dysentery, gonorrhea, tuberculosis, rubella, mumps and other infections, mainly intestinal, genitourinary);
- hereditary causes;
- metabolic disorders (gout, diabetes);
- autoimmune diseases (rheumatoid arthritis, systemic lupus erythematosus, psoriasis);
- overheating, hypothermia, prolonged exposure to the sun;
- decompensated and excessive physical activity;
- overweight;
- insufficient or unbalanced diet (deficiency of protein, calcium, essential amino acids and antioxidants), as well as dehydration;
- smoking and other bad habits.
As a rule, the development of polyarthritis is promoted not by one, but by several reasons at once; in some cases, the etiology of the disease remains unclear (for example, in juvenile idiopathic polyarthritis, which occurs in children aged 16 years).
Often the symptoms of polyarthritis resemble those of rheumatoid arthritis, which most often affects women aged 30-35 years. These diseases combine pain and stiffness in the joints, increased fatigue, swelling and redness of the skin, rash over the sore spot, high body temperature, loss of appetite and body weight. However, the directions of therapy vary - that is why the treatment of polyarthritis of the joints should be selected by a doctor who is able to establish its true cause.
There are no specific signs and treatment of polyarthritis in women and men, but scientists have found that:
- women are more likely to suffer from rheumatoid arthritis because their bodies produce more antibodies;
- Metabolic, in particular gouty, polyarthritis affects men almost 20 times more often.
Diagnosis of polyarthritis, as a rule, begins with laboratory blood tests, which make it possible to determine whether the patient has a seropositive (antibodies to the body’s own cells are present in the blood) or seronegative (“wrong” antibodies are absent) form of the disease.
How to search for the right specialist?
First, you need to contact the reception desk of a medical institution and try to find out which doctor to see for arthrosis or arthritis. But usually it is not possible to find out. Then you need to try the following: you can make an appointment with a therapist, and then find out from him which doctor treats arthrosis. But this will be quite difficult to do, since there are usually large queues of patients outside the therapist’s office. Therefore, you will have to spend the whole day finding out.
In some clinics, diseases such as polyarthritis, rheumatoid arthritis, and glenohumeral periarthritis are for some reason treated by a therapist. But this is the wrong solution to the problem, since the doctor of this plan has a generalized specialization and cannot know all the nuances of such ailments as arthritis or arthrosis. The therapist should simply send various patients to more specialized specialists, and not treat them.
What is the difference between arthritis and arthrosis in the video:
You can go to a private clinic, where it is very easy to find out which doctor you should go to to cure arthritis and arthrosis. There, appropriate care and monitoring of the patient will be provided. But for this you need to have appropriate financial support, which not every patient has.
Since these diseases tend to most often develop in people over 35 years of age, every person who has reached this age must be prepared and find out in advance which specialist he should visit if symptoms of this disease appear.
Stages of polyarthritis of joints
The division of the inflammatory process into stages in polyarthritis has a practical justification: each stage has its own risks, differences in the drug treatment of polyarthritis and the intensity of therapy.
To diagnose polyarthritis and determine the stages, X-ray examination of diseased joints, ultrasound, and, if necessary, CT and MRI are used. You may also need to take blood and joint fluid for laboratory testing and arthroscopy. Determination of biochemical signs for the treatment of polyarthritis plays a key role.
Stage 1 polyarthritis
Regardless of the cause, the symptoms of polyarthritis demonstrate minimal disease activity:
- pain is mild or moderate;
- noticeable swelling is usually absent;
- there is slight morning stiffness in the joints;
- muscle endurance decreases, which is attributed to ordinary fatigue;
- Occasionally, patients may experience seizures.
Discomfort at rest, as a rule, is not noted by patients as a pathology, so they do not think about the symptoms and treatment of polyarthritis. Signs of the disease may appear sporadically - for example, when the weather changes or after exercise - and disappear without taking medications for polyarthritis of the joints.
When visiting a doctor at the first stage of the disease, 9 out of 10 patients are cured! In those patients in whom the pathology becomes chronic, adequate treatment of polyarthritis can reduce health risks, improve quality of life, and slow down the destruction of joints.
Stage 2 polyarthritis
At this stage, obvious signs of polyarthritis are observed:
- the patient feels acute pain when moving, dull, aching or bursting pain when at rest;
- swelling;
- joint stiffness, clearly noticeable when performing everyday movements;
- increased local or general body temperature;
- muscle atrophy and deformation of the affected joints begin.
Stage 3 polyarthritis
The last stage of the disease leads to disability and incapacity for the patient, even if he receives constant drug treatment for polyarthritis. It is characterized by:
- severe pain that torments the patient even at rest and does not go away during remission;
- signs of an acute inflammatory process (fever, weight loss, decreased mood and appetite);
- serious restrictions of mobility in the joints and their deformation with swelling.
In some types of polyarthritis of the joints at this stage, serious damage to the respiratory, cardiovascular, digestive and other internal organ systems occurs.
Traditional methods
In the treatment of polyarthritis, folk recipes can also be used; such therapy is allowed only after consultation with the attending physician. Modern medicine has a large number of recipes; tinctures, compresses, lotions, decoctions, etc. are used as part of treatment.
Effective recipes:
- applying burdock and cabbage leaves at night;
- taking birch sap;
- pine baths;
- rubbing cinquefoil tincture or eucalyptus oil;
- compresses from chamomile and sweet clover decoctions.
The combination of all of these methods of influencing the pathology will help ensure long-term remission and prevent deterioration of the condition.
Treatment of polyarthritis
Polyarthritis of the joints, which is associated with modifiable factors (lifestyle, consequences of non-chronic infectious diseases), has a high chance of a complete cure for the patient. If polyarthritis is secondary and associated with chronic diseases (rheumatoid arthritis, psoriasis), the patient requires lifelong therapy for the underlying disease and prevention of exacerbations of the joints.
Complex therapy of polyarthritis itself includes measures to eliminate pain and relieve inflammation, activate metabolic processes and regenerate cartilage tissue in diseased joints. In addition to pharmacotherapy and physiotherapy, these include control of diet and body weight, normalization of sleep and exercise, and the use of orthoses.
Before treating polyarthritis, the doctor needs to determine the stage of the inflammatory process - whether it is in the stage of exacerbation or remission. This is due to the fact that in the acute phase of the disease, massage, exercise therapy and some physiotherapeutic techniques are contraindicated and are replaced by anti-inflammatory drugs for polyarthritis of the joints.
Physiotherapy for polyarthritis of joints
In the absence of contraindications, patients with signs of polyarthritis are prescribed:
- magnetic therapy;
- laser therapy;
- acupuncture;
- electrophoresis with drugs for polyarthritis;
- amplipulse;
- thermotherapy (heating applications, cryotherapy, etc.);
- UV therapy;
- ultrasound therapy;
- UHF;
- barotherapy;
- balneological techniques (herbal, radon, bromine and other baths) and mud therapy.
Massage for polyarthritis of joints
In the absence of acute inflammation, patients with polyarthritis can attend therapeutic massage sessions, which prevent muscle atrophy and improve metabolic processes in the joint. But some massage movements can be repeated at home, on your own:
- Superficial rubbing movements (circular, back and forth) - repeat until the skin becomes noticeably warm.
- Stretching movements (for example, with the edge of the palm) designed to gently stretch muscles and ligaments without injuring them at the points of attachment to the articular heads.
- Deep kneading movements (mainly with fingertips).
Exercise therapy in the treatment of polyarthritis
Therapeutic exercises are effective for relieving inflammation, nourishing and regenerating cartilage and periarticular tissues, and reducing pain.
Exercise therapy exercises for the treatment of polyarthritis of the joints are performed daily, at least 3 times a day for 15 minutes. This helps to consolidate the results of medications and physical therapy and bring the disease into stable drug-free remission.
An individual list of exercises, taking into account the patient’s age, gender, physical fitness, stage of the disease and lifestyle, should be compiled by a specialist - exercise therapy instructor, rehabilitation specialist.
What specialty should you look for?
Since the disease has many subtypes, the symptoms of which are mainly manifested by severe pain, you need to know that there is no clear answer to the question about the specialty of the doctor for the treatment of such diseases. The disease can have the following types:
- Arthritis of the fingers or joints of the feet.
- When damage occurs in the shoulder area, glenohumeral periarthritis occurs.
- Rheumatoid arthritis is common in many patients.
- If the lesions are multiple in the arms and legs, then you will need a doctor who treats polyarthritis.
Therefore, to eliminate the ailments that have arisen, doctors of different specialties and areas are usually required. This depends on the root cause of the disease, the presence of old injuries in the patient, and pathological changes in the joints. Therefore, it is necessary to distribute specialists over time while simultaneously separating them according to specific symptoms of the disease and its subtypes.
Based on this, any patient with arthritis or arthrosis can seek help from specialists such as an orthopedist, rheumatologist, traumatologist or surgeon. In some large treatment centers and clinics that have large staffs of medical specialists, you can find an arthrologist who is able to cope with the above types of arthritis. But you shouldn’t count on this, since such a specialty is quite rare for most cities and the clinics located in them.
Medicines for the treatment of polyarthritis
Drug treatment of polyarthritis includes taking anti-inflammatory and painkillers, chondroprotectors, blood microcirculation correctors and angioprotectors, vitamins and minerals. Depending on the cause of the disease, effective drug treatment of polyarthritis may also require immunosuppressive, antihistamine and/or antibiotic therapy. Based on the patient’s psycho-emotional state, the doctor may also prescribe antidepressants.
Chondroprotectors for polyarthritis
These drugs for the treatment of polyarthritis are aimed at eliminating not the symptoms, but the consequences of the disease - they start the process of regeneration of synovial cartilage in the joint, slow down its decay and deformation of the joint. The effect after taking chondroprotectors occurs within 3-6 months. To maintain joints, doctors recommend lifelong use of glucosamine and chondroitin sulfate in courses of about 6 months a year.
Effective chondroprotectors include: artracam, dona, movex, chondros, structum, alflutop, artiflex, elbona, protecon, chondroitin complex and others.
Anti-inflammatory for polyarthritis
Anti-inflammatory drugs in the treatment of polyarthritis are used externally, orally, intravenously, intramuscularly or in the form of intra-articular injections (in this case they can be combined with anesthetics, hyaluronic acid preparations, antibiotics).
In the early stages, with a mild or moderate course of the disease, non-steroidal anti-inflammatory drugs for polyarthritis of the joints (NSAIDs) are prescribed: ibuprofen, ketoprofen, diclofenac, meloxicam, piroxicam, nimesulide, voltaren, indomethacin, naproxen.
If NSAIDs are not enough to cope with the symptoms of the disease, glucocorticosteroid drugs are used to treat polyarthritis: prednisolone, methylprednisolone, betamethasone, Maxitrol, Metypred, Kenalog, Clenil, hydrocortisone.
NSAIDs are often combined with gastrointestinal protective agents (for example, omeprazole).
Immunosuppressants for polyarthritis
For rheumatoid polyarthritis, the so-called basic therapy with drugs for polyarthritis that suppress the activity of the immune system. These include: methotrexate, sulfasalazine, xeloda, azathioprine, leflunomide, ftorafur and others.
Attention: taking these medications for polyarthritis of the joints must be suspended during colds and other illnesses.
Auxiliary agents in the treatment of polyarthritis
To relieve symptoms and normal nutrition of periarticular tissues, drugs that protect blood vessels and relax muscles are used in the treatment of polyarthritis of the joints.
Antispasmodics and muscle relaxants: mydocalm, papaverine, no-shpa, sirdalud (tizanidine), Novigan, baclosan, tolperisone and others.
Angioprotective drugs for polyarthritis: troxerutin, troxevasin, horse chestnut extract, detralex, actovegin, pentoxifylline.
What to do if there is no arthrologist in the medical institution?
For any person with problems with the described disease, an effective solution may be the following: one should alternately visit specialists of different profiles who can alleviate the patient’s situation at different stages of the treatment process.
To do this, it is best to visit a surgeon first.
He examines the tissues and joints and gives his conclusion, with which the patient is sent to a rheumatologist. The doctor of this specialty is the main one in the fight against arthritis. He makes the main appointments, conducts consultations with the patient, supervises the patient until the end of the treatment process.
If the surgeon has concluded that the underlying disease has developed due to old or new injuries, then a traumatologist will be needed to eliminate the symptoms of the disease and the causes that led to its appearance. After this specialist completes the course of therapy, the patient goes under the care of a rheumatologist, who eliminates all other signs of the disease.
Read also: Joint diseases
If the main course of treatment is successfully completed, the patient may be referred to an orthopedist, as special shoes or pads may be needed. This usually occurs during the period of rehabilitation and recovery of a person after treatment for arthritis or arthrosis. The disease may have relapses; in this case, you should check with a rheumatologist every six months.
In severe cases of arthritis, most often the surgeon directly prescribes an operation, after which the patient goes under the care of a rheumatologist, orthopedist and traumatologist. Recovery and rehabilitation of the patient after surgery is carried out by doctors of these particular specialties.
Why is polyosteoarthritis dangerous?
Multiple joint lesions indicate serious disorders in the body. As a rule, the disease develops against the background of other pathological conditions, and does not become a consequence of an accidental injury, therefore the prognosis is always less favorable than with localized osteoarthritis of the elbow, knee or hip joint.
Among the most common complications is limited mobility of the limbs and spinal column. If the disease is not treated at all, the joints wear out to such an extent that every movement brings incredible pain. And since the lesions are multiple, disability is one step away.
Prevention
To prevent polyarthritis, it is necessary to lead a healthy lifestyle: eat right, exercise, and get rid of bad habits. Regular physical activity will help strengthen your muscles and joints. A good way to prevent polyarthritis is swimming. Take a walk in the fresh air every day, walk more. Stop smoking.
Hardening plays a decisive role in the prevention of polyarthritis. You can avoid the manifestations of the disease thanks to cold douches, rubdowns and water procedures with a gradual decrease in temperature to 18 degrees.
It is important to avoid traumatic situations and treat all infectious diseases in a timely manner. At the first symptoms, you should consult a doctor for examination and treatment.
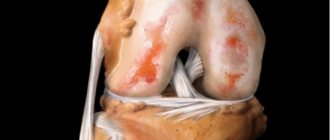
Pathogenesis
Polyarthritis originates in the tissues of the body and in the blood vessel system. Rapidly progressive areas of inflammation extend to the cartilage, joint capsule and ligaments. As a result, the joint becomes deformed, causing acute pain to the patient.
Rheumatoid arthritis is based on a chronic inflammatory process in the lining of the joints, caused by the development of a local immune reaction. Under the influence of various factors, the immune system begins to attack the body's tissues, perceiving them as a foreign object. The defense fails, and the brain mistakenly sends a signal to the body about danger.